Read Bio
Since 1979, Dov Apfel has been passionate about advocating for birth injury and medical malpractice victims. Mr. Apfel’s career-long record of achievements in birth injury litigation, education, and advocacy has been recognized by the Executive Board of the Birth Trauma Litigation Group of the American Association for Justice. His expertise is demonstrated by his numerous awards, presentations on birth injury topics at legal conferences for organizations like the AAJ and ATLA, and articles published by Trial Magazine and many others.
Read Bio
Since 1979, Dov Apfel has been passionate about advocating for birth injury and medical malpractice victims. Mr. Apfel’s career-long record of achievements in birth injury litigation, education, and advocacy has been recognized by the Executive Board of the Birth Trauma Litigation Group of the American Association for Justice. His expertise is demonstrated by his numerous awards, presentations on birth injury topics at legal conferences for organizations like the AAJ and ATLA, and articles published by Trial Magazine and many others.
Key Takeaways
Cooling therapy lowers a baby’s body temperature to prevent further brain damage after oxygen deprivation (HIE). This treatment significantly improves survival rates and reduces the risk of severe disabilities like cerebral palsy and blindness.
Cooling therapy must begin within six hours of birth to be effective. The sooner it starts, the better the outcome. Delays in diagnosis and treatment can worsen brain injury and lead to lifelong consequences.
HIE is often caused by preventable medical errors, such as failure to perform a timely C-section or monitor the baby’s distress. Families may be eligible for legal compensation to cover long-term care and hold healthcare providers accountable.
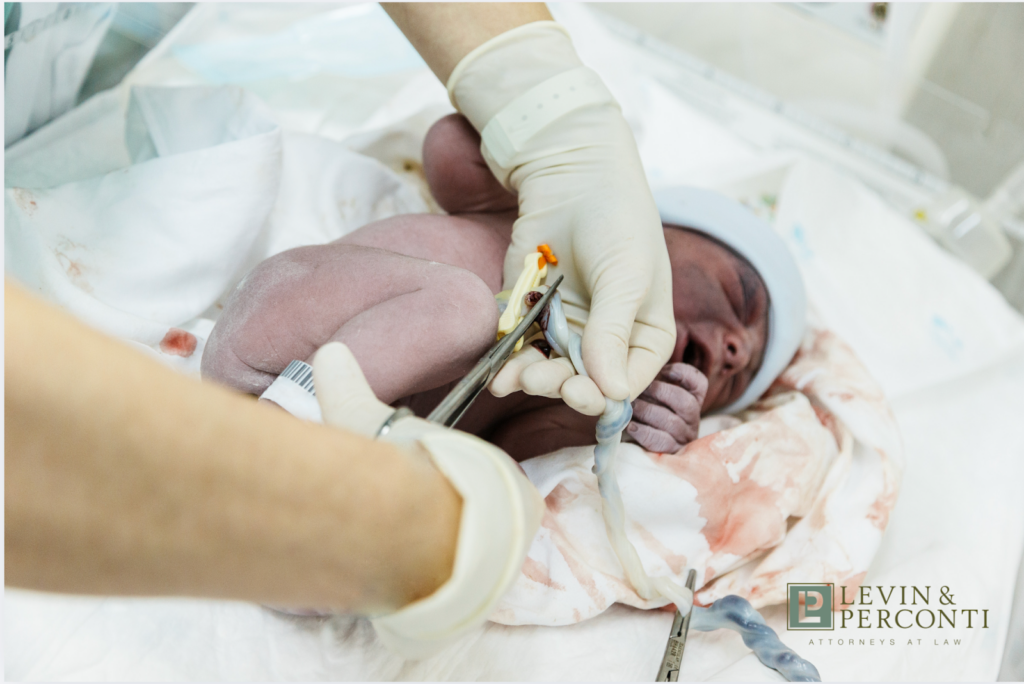
Hypoxic-ischemic encephalopathy, or HIE, is a devastating medical condition affecting newborns after a traumatic birth. It occurs when the infant’s brain is deprived of oxygen and blood flow. Hypoxic means insufficient oxygen, ischemic means lack of blood flow, and encephalopathy means an alteration in brain function. This condition is also known as neonatal encephalopathy.
HIE occurs in phases that begin with the initial injury, known as primary energy failure. This is followed by a latent period during which oxygen and blood flow are restored, and the brain resumes normal metabolism. This period generally concludes approximately six hours after the initial injury.
The damage from primary energy failure causes the baby’s brain to absorb blood and oxygen too quickly. This condition is known as reperfusion injury or secondary energy failure and can be more damaging than the first. The latency phase provides a brief window of opportunity for administering cooling therapy.
What Is HIE Cooling Therapy?
HIE cooling therapy involves gradually reducing an infant’s head or body temperature to 92 degrees Fahrenheit to slow the brain’s metabolism and prevent further chemical damage. This temperature is maintained for 72 hours, followed by a gradual rewarming period. HIE cooling therapy is only effective if cooling is achieved within six hours of birth.
HIE cooling therapy is a standard of care in newborns with moderate and severe HIE because they frequently experience reperfusion injury. The severity of HIE is measured using the Sarnat scoring model to define the stages of HIE, with mild HIE designated as Stage 1 and severe HIE as Stage 3.
A study published by Pediatric Research found that 16 percent of untreated children with mild HIE experienced disability at 18 to 22 months, and 40 percent had language deficiencies. According to the study, approximately 75 percent of hospitals in the United Kingdom use cooling in cases of mild HIE with varying methodologies.
What Are the Benefits of Cooling Therapy?
Cooling therapy may reduce mortality and the development of severe disabilities. A systematic review of 11 randomized controlled trials by the Cochrane Neonatal Review Group found statistically significant improvements in mortality and major neurodevelopmental disability at 18 months of age with minimal side effects.
A study published by the New England Journal of Medicine found the following improvements in babies who received HIE hypothermia therapy:
- 24 percent mortality compared to 37 percent who did not receive cooling therapy
- 19 percent occurrence of cerebral palsy compared to 30 percent in the non-cooled group
- 44 percent occurrence of moderate to severe disability compared to 62 percent in the non-cooled group
- 7 percent incidence of blindness compared to 14 percent in the non-hypothermia group
What Is the Goal of Cooling Therapy?
HIE cooling therapy aims to prevent reperfusion injury by slowing the brain’s oxygen consumption and giving it more time to recover from the initial injury. If reperfusion injury is successfully abated, the baby is more likely to survive and recover without severe neurodevelopmental disabilities.
If reperfusion injury is not prevented, the secondary energy failure phase will begin approximately 12 to 36 hours after the initial injury and may last seven to 14 days. This results in a worsening of HIE through the following mechanisms:
- Continued cell death
- Failure of the mitochondria, the energy centers of the cells
- Accumulation of fluids in the brain cells, resulting in swelling
- The release of excitatory amino acids, resulting in the release of toxic free radicals and cell death
The Cochrane analysis found that preventing the secondary phase of HIE through cooling therapy resulted in a statistically significant reduction of mortality and neurodevelopmental disabilities.
When Should Cooling Therapy be Initiated?
It is crucial that an infant is cooled to the target temperature of 92 to 94 degrees Fahrenheit within six hours of the initial injury and before the latent period has concluded. However, six hours is a maximum.
According to the California Perinatal Quality Care Collaborative, the latency period may be shorter in severe HIE, and therapeutic hypothermia was more effective when initiated an hour and a half following the injury compared to five-and-a-half hours later. It was not effective when administered after eight-and-a-half hours.
In the Total Body Hypothermia trial, infants received the most benefit when treatment commenced within four hours.
What Happens During HIE Cooling Treatment?
During HIE cooling therapy, the infant is gradually cooled and maintained at approximately 92 degrees for 72 hours, then gradually rewarmed. This must occur in a Level III or Level IV neonatal intensive care unit with the appropriate equipment for active cooling and the ability to closely monitor the baby’s responses to treatment and provide support as needed.
Monitoring and support must include the following:
- Respiratory support – assisted ventilation, frequent saline suction, and oxygen supplementation
- Positioning and skin care – frequent repositioning to prevent bedsores
- Cardiovascular support – heart monitoring and administration of drugs to regulate heartbeat as needed
- Fluid and electrolyte management – monitoring of kidney function, glucose, and electrolytes with replacement as needed
- Restriction of feeding during therapy
- Sedation – as needed to prevent distress during cooling
- Blood coagulation – monitoring and providing plasma supplementation as needed to prevent blood clots
HIE hypothermia therapy is administered through the use of active cooling, but if transport to an appropriately equipped NICU is necessary, passive cooling may be used to ensure the baby’s core temperature is reduced before the window of opportunity passes.
Active Cooling
Active cooling involves using a special blanket through which water circulates to gradually cool the baby. A temperature probe is placed in the baby’s rectum or esophagus. This may be connected to the cooling blanket to facilitate communication between the devices.
Intravenous lines may be placed through the abdomen where the umbilical cord was attached. This allows the NICU to provide fluids, draw blood, and monitor oxygen. An EEG machine will be attached to monitor for seizures.
The baby’s body temperature will slowly be lowered to 33.5 degrees Celsius, or 92.3 degrees Fahrenheit. After 72 hours, the infant is gradually rewarmed through the circulation of warm water through the cooling blanket.
Selective Head Cooling
Therapeutic benefits may be achieved through selective head cooling. According to the Ann & Robert H. Lurie Children’s Hospital of Chicago, an FDA-approved cap known as a Cool-Cap may be fitted to the infant’s head, through which water circulates to gradually cool the head for 72 hours, after which warmer water is circulated through the device to gradually warm the infant.
According to the Canadian Pediatric Society, selective head cooling and full-body cooling yield similar therapeutic benefits and patient outcomes.
Passive Cooling
Passive cooling is implemented when an infant with HIE must be transported to a Level III or Level IV NICU for cooling therapy. Due to the short time window for commencing treatment, passive cooling is often necessary to achieve the target temperature before the latent period ends.
During passive cooling, heat sources are removed, and the infant is kept in as cold an environment as possible leading up to and during transport. The rectal temperature is monitored every 15 minutes.
One of the risks of passive cooling is overcooling because continuous monitoring equipment is unavailable, and it may be difficult to control ambient temperatures. However, according to the Journal of Perinatology, the benefits may outweigh the risks. Passive cooling may be the only way to ensure the reduced temperature is achieved on time to improve the infant’s outcome.
Is There an Alternative to Passive Cooling during Transport?
Servo-controlled active cooling employs gel packs to facilitate cooling during transport, which may be a superior alternative to passive cooling. According to Acta Paediatrica, an international medical journal, infants who received servo-controlled active cooling more reliably arrived at the NICU having achieved the optimal temperature range. However, any cooling was superior to no cooling.
Eligibility Criteria for HIE Hypothermia Therapy
HIE hypothermia therapy has only been proven safe and effective for infants that meet the following criteria, according to the Journal of Clinical Neonatology:
- Born at 36 weeks gestation or later
- Evidence of hypoxia during birth
- At least two of the following:
- Apgar score of 5 or less 10 minutes after birth
- Mechanical ventilation or ongoing resuscitation 10 minutes after birth
- A diagnosis of metabolic or mixed acidosis
- The presence of seizures (an automatic inclusion with or without other inclusive criteria)
- EEG evidence of encephalopathy
- Diagnosis of moderate to severe encephalopathy based on physical examination
Infants are not eligible for treatment if they have any of the following characteristics:
- Premature birth, which is before 35 weeks of gestation
- Birth weight of less than 4.4 pounds
- Therapy not initiated within 6 hours
- Suspected blood clotting disorder
- Life-threatening cardiovascular or respiratory symptoms
- Significant congenital malformations
- Imperforate anus, meaning the anus is missing or blocked
- Suspected neuromuscular disorders
- Chromosomal anomalies that may be fatal
- A determination that death is inevitable
If an esophageal probe is used, HIE may be an option for a child with an imperforate anus.
Persistent pulmonary hypertension has excluded newborns from cooling therapy in the past. However, according to the Journal of Clinical Neonatology, multiple studies have found no difference in the incidence of persistent pulmonary hypertension between infants who were cooled and those who were not, and cooling neither worsened nor induced it.
Limited data suggest that cooling therapy may benefit preterm infants born at 34-35 weeks. While the risks of complications are higher, a study published in the Journal of Pediatrics concluded therapy may be “feasible” for these newborns. However, more research is needed to draw a definitive conclusion.
How Long Can Cooling Therapy Last?
HIE cooling therapy is administered for 72 hours. According to the Canadian Pediatric Society, longer periods of hypothermia have not yielded additional benefits.
What happens after HIE cooling treatment?
After 72 hours, the infant is gradually warmed to a normal body temperature. Ideally, this should occur over six to 12 hours. Rewarming generally occurs at a rate of approximately 0.9 degrees per hour to about 97.7 degrees Fahrenheit.
The rewarming phase requires continuous monitoring of the following:
- Blood pressure
- Heart rate
- Respiratory rate
- Oxygen saturation
- Blood glucose
- Blood counts
- Arterial blood gas
Blood pressure is expected to decrease as the baby’s temperature rises due to a reduction in blood flow resistance in blood vessels at warmer temperatures. An increase in heart rate is also expected.
A decrease in urine output and electrolyte imbalances are also expected due to kidney clearance rate changes.
In some cases, seizures and a worsening of encephalopathy may occur. Under these circumstances, recooling for 24 hours is recommended, after which rewarming can resume.
Whether or not HIE cooling therapy is successful, your child may receive comprehensive follow-up care through a multidisciplinary specialty team after discharge, according to Lurie Children’s Hospital of Chicago. This team may be comprised of the following specialists:
- Neonatologist
- Developmental pediatrician
- Neurologists
- Occupational therapists
- Physical therapists
- Speech therapists
Risks and Complications of Cooling Therapy for HIE
While HIE cooling therapy is generally safe and effective, the procedure has risks. Complications may occur during cooling or rewarming. Complications are not always preventable, but careful monitoring is crucial in minimizing their effects.
The following complications may arise as a result of cooling therapy:
- Bedsores due to cold skin and edema
- Displacement of blood water into the tissues, known as hypovolemia
- Kidney impairment following treatment
- High sodium levels during the rewarming phase
- Increased risk of necrotizing enterocolitis, a deadly gastrointestinal condition most commonly affecting premature infants who consume formula
- Distress from cooling, which could negate the therapeutic effects of hypothermia
- Blood clots
- Slowed metabolism of drugs by the liver
- A threefold risk of seizures during rewarming, doubling the likelihood of death or development of a neurological disability by age 2
- Ventricular arrhythmias
- Bradycardia, or slow heart rate
- Hypotension
- Reduced cardiac output
- Increased oxygen consumption
- Infection, including sepsis
- Feeding intolerance and delayed digestion
How Can Levin & Perconti Help?
Our hypoxic-ischemic encephalopathy lawyers are experienced medical malpractice attorneys with more than 200 years of combined experience helping parents recover substantial compensation for HIE and other birth injuries stemming from medical negligence.
Hypoxic-ischemic encephalopathy is often preventable. In many cases, it results from a birth injury caused by medical malpractice. Medical malpractice occurs when a health care provider fails to provide a reasonable standard of care, causing an injury to the patient.
The following medical errors may cause HIE:
- Failure to perform a timely C-section
- Failure to adequately monitor fetal distress
- Lack of communication by delivery room personnel
- Failure to properly and timely respond to emergency complications
- Failure to monitor or diagnose pregnancy risk factors
- Improper administration of anesthesia or other medications
A physician’s failure to timely diagnose HIE and initiate cooling therapy may exacerbate the injury. Failure to adequately monitor the baby during cooling therapy and the rewarming phase can allow the baby to suffer a further preventable injury.
If your child has been diagnosed with HIE with subsequent disabilities, you may be eligible to recover substantial compensation. We have helped parents of infants with HIE recover millions of dollars in settlements and verdicts, including the following:
- $40 million verdict on behalf of the now 19-year-old woman who suffered a severe and permanent brain injury during birth due to a delayed C-Section delivery
- $27 million verdict on behalf of a child who suffered preventable HIE and asphyxia injuries at birth, resulting in permanent cognitive and developmental impairments
- $11.5 million settlement for a child born at the U.S. Naval Hospital in Guam who suffered a catastrophic hypoxic-ischemic brain injury from negligent neonatal resuscitation and intubation
- $6.5 million for a child who suffered a brain injury after a hospital failed to provide appropriately trained staff to perform a neonatal resuscitation
- $6.5 million settlement for a girl who suffered a brain injury at birth and developed cerebral palsy after physicians failed to perform a timely Caesarian
- $3.5 million settlement to the family of a baby who died from multiple complications stemming from a hypoxic-ischemic brain
We consistently achieve successful results while providing compassionate, fervent advocacy with personalized attention to each client. If your child has died or developed disabilities from HIE, we can help you hold the negligent health care providers accountable. Contact us today for a free consultation.