Umbilical Cord Compression
The umbilical cord is the baby’s lifeline during pregnancy. It delivers oxygen, blood, and vital nutrients to the developing fetus, ensuring that it grows to term without issue. It also transports the fetus’ waste to the placenta.
Quick Links
- What Are the Causes of Umbilical Cord Compression?
- What Are the Risk Factors of Umbilical Cord Compression?
- What Are the Dangers of Cord Compression?
- Cerebral Palsy
- How Does One Treat Umbilical Cord Compression?
- Treatment Options for Mild Cases of Compression
- Treatment Options for Moderate Cases of Compression
- Treatment Options for Severe Cases of Compression
- What Are My Legal Options for Umbilical Cord Compression Injuries?
- Testimonials
The umbilical cord can become compressed when the baby’s weight, the vaginal walls, or the placenta strain the cord during pregnancy, labor, or delivery. Cord compression can restrict blood flow and oxygen to the baby, risking fetal malnourishment, brain damage, or even death. While doctors can easily recognize this condition, treating it promptly is vital.
Umbilical cord compression is relatively common in the U.S. The American Pregnancy Association found that about one in every ten deliveries involves a compressed umbilical cord.
What Are the Causes of Umbilical Cord Compression?
There are four leading causes of umbilical cord compression, including:
Prolapse into the Cervix
Prolapse is a common cause of umbilical cord compression, occurring in between 1.4 and 6.2 per 1000 pregnancies. In cases of prolapse, the umbilical cord slips into the birth canal after the membranes have ruptured (more commonly referred to as the mother’s “water breaking”) but before the baby has descended into the canal. As the fetus lowers, they may compress the cord, reducing or cutting off the fetus’ oxygen supply. This condition poses a significant danger to the infant.
Nuchal Cord
A nuchal cord is a condition in which the umbilical cord wraps around the baby’s neck. When the umbilical cord is an average length (50-60 centimeters), a nuchal cord may not pose any problems. This condition is more likely when the cord is longer than 60 cm.
Knotted Cord
In less than 2% of pregnancies, the umbilical cord can become knotted as the fetus moves in the womb. While not inherently dangerous, a knotted cord can present a problem if it becomes too tight. As the fetus continues to move, the knot may become tighter, worsening the compression.
Uterine Contractions
Cord compression happens naturally and temporarily during uterine contractions. In cases of umbilical cord compression, the extent of the compression determines the severity of the damage to the baby. Most often, the fetus can continue to develop normally through all the trimesters. However, in some instances, the baby may need medical attention. Doctors must approach each unique instance with care and precision.
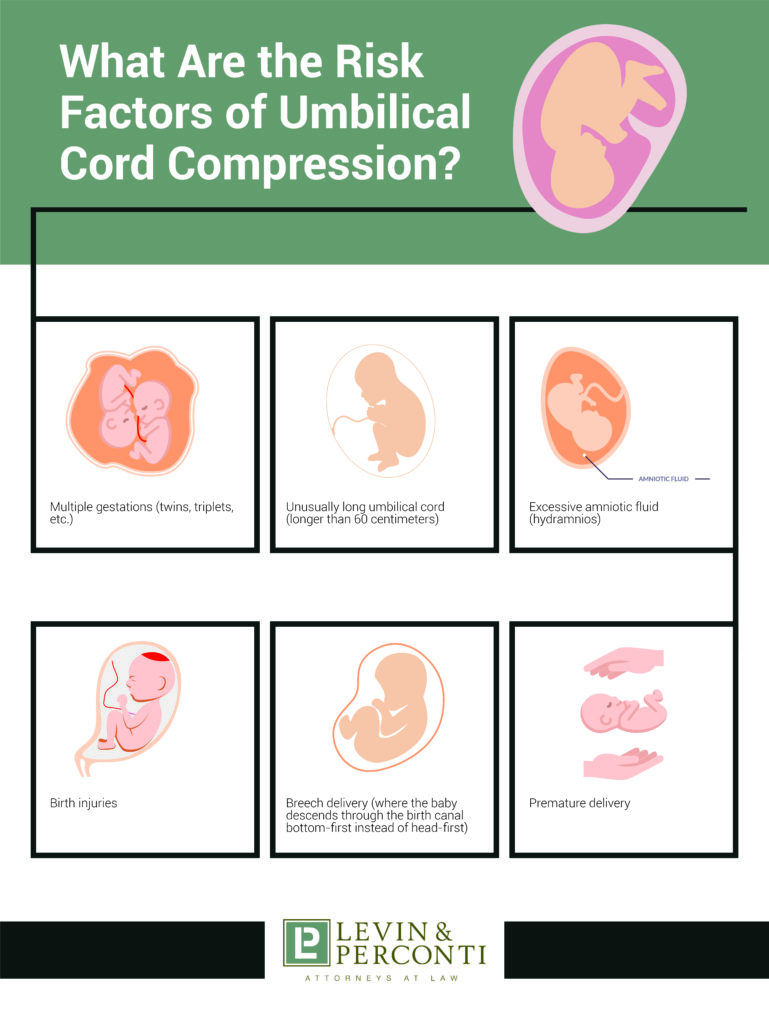
What Are the Risk Factors of Umbilical Cord Compression?
Several factors that may increase the likelihood of umbilical cord compression include:
- Multiple gestations (twins, triplets, etc.)
- Unusually long umbilical cord (longer than 60 centimeters)
- Excessive amniotic fluid (hydramnios)
- Birth injuries
- Breech delivery (where the baby descends through the birth canal bottom-first instead of head-first)
- Premature delivery
Some positions of the fetus in the womb can contribute to umbilical cord compression, such as:
- Unstable lie: The baby moves and shifts continuously in the last 14-21 days of the pregnancy.
- Oblique lie: The baby’s head is near the hip, and their head and body are diagonal in the mother’s pelvis.
- Traverse lie: The baby’s trunk, arm, or shoulder faces the birth canal (the baby is “sideways” in the birth canal).
What Are the Dangers of Cord Compression?
A compressed umbilical cord can restrict blood and oxygen flow to the baby, which in turn causes medical conditions known as ischemia and hypoxia. Detecting umbilical cord compression soon enough should allow the doctor to deliver the baby without any lasting impact. However, if the doctor fails to diagnose or treat the condition, the baby may experience severe and lasting harm, including:
- Behavioral disorders
- Brain damage and associated physical issues
- Fetal heart abnormalities
- Poor physical development
Cerebral Palsy
Because umbilical cord compression can restrict oxygen to the fetus, it can cause brain damage which sometimes leads to cerebral palsy. Every year, about 10,000 babies are born with some form of cerebral palsy, though many cases are not diagnosed until 1-2 years after birth. Symptoms include stiff muscles, missed developmental milestones, floppy muscle tone, or abnormal movement.
There’s no known cure for cerebral palsy — this condition does not progress or heal with age — but its symptoms are manageable. In particular, physical therapy can reduce pain and muscle spasms.
How Does One Treat Umbilical Cord Compression?
After identifying the compressed part of the umbilical cord, your physician should treat you quickly to prevent further complications. Treatment of umbilical cord compression considers the compression’s underlying cause, the baby’s current health status, and the risk posed to the baby’s condition.
Treatment Options for Mild Cases of Compression
For mild cases of compression (where the baby appears to be in stable condition), physicians often suggest:
- Oxygen Administration: Receiving supplemental oxygen can help normalize the baby’s heart rate and prevent further compression.
- Changing the Mother’s Position: Sometimes, switching to another position can relieve compression and get more blood flowing to the fetus.
Treatment Options for Moderate Cases of Compression
In more moderate cases, doctors may propose the following treatment options:
- Intravenous (IV) Fluids: When compression slows down nutrient delivery, hydration via IV can help nourish the baby.
- Medication to Stop Contractions: During labor, the doctor may decide to delay contractions. In some instances this can help the baby recover before delivery, and it can also resolve umbilical cord compression.
Treatment Options for Severe Cases of Compression
In severe cases where there are signs of fetal distress, doctors typically suggest more aggressive treatment measures. These include:
- Amnioinfusion: If amniotic fluid is low, a doctor might recommend amnioinfusion. This procedure involves using a saline solution to open up the veins and arteries in the uterus.
- Manually adjusting a Prolapsed Cord or Nuchal Cord: Depending on the stage of the mother’s pregnancy, the position of the umbilical cord, and other relevant risk factors, it may be possible to resolve a prolapsed or nuchal cord manually.
- C-Section Delivery: If there are signs that the baby is in danger, a C-section may be necessary to save their life.
What Are My Legal Options for Umbilical Cord Compression Injuries?
There are often steps that physicians can take to prevent complications resulting from compressed umbilical cords. If you suspect that you suffered these complications due to medical negligence, you might be eligible for compensation.
Some examples of compression-related conditions for which families can earn compensation include:
- Cognitive or behavioral disorders
- Cerebral palsy
- Birth asphyxia
- Fetal acidosis
- Hypoxic-ischemic encephalopathy (HIE)
- Developmental disabilities
- Stillbirth
Each case is unique, but these are some damages you can recover in a birth injury lawsuit:
- Loss of consortium (often called “loss of comfort”)
- Out-of-pocket costs (e.g., purchasing assistive devices, or other equipment needed throughout your child’s life)
- Pain and suffering
- Medical expenses
- Funeral expenses
At Levin & Perconti, we work tirelessly to help you and your family receive the compensation you need to help your child heal from their injuries and suffering. We hold the responsible parties accountable for their negligent or wrongful actions to prevent future injuries to other families and their newborns.
Our birth injury team is led by Dov Apfel, who is nationally recognized for his child advocacy. We have successfully recovered numerous favorable results in birth injury and medical malpractice lawsuits over the years, including:
$14 Million
Settlement
for the family of a child who suffered brain injury due to lack of oxygen during her birth. Despite nonreactive fetal heart tracings, the Chicago area hospital failed to promptly respond to fetal monitoring and did not arrange for a C-section in a timely manner
$11.5 Million
Settlement
FTCA settlement for a child born at the U.S. Naval Hospital in Guam who suffered a catastrophic hypoxic-ischemic brain injury as a result of a negligent neonatal resuscitation and intubation. Parents were both active duty at the time
$9 Million
Settlement
to the family of a baby who suffered permanent brain damage as a result of a doctor’s failure to test the mother for Group B Strep Meningitis during prenatal care
Don’t wait to pursue justice. Get help today. Contact us now for a free case evaluation.
Testimonials
Not only were they so professional but also so caring and thoughtful. It was very difficult going over the facts in our mother's case but they were so compassionate and understanding and allowed us to be with them every step of the way. We were able to sit in on the depositions and we were really able to see how hard they worked on our behalf.
During that time, my family and I suffered the loss of my mother. Mr. Levin and Mr. Perconti were more than just our lawyers. Words can’t really express our gratitude.
They were most patient and responded timely to many questions throughout the entire process. All demonstrated professionalism and extensive knowledge of case and state laws. Their in-depth investigative work uncovered details which were unknown to us and yet sadly confirmed our suspicions. We would recommend the Levin and Perconti Law firm and especially this team.
During that time, my family and I suffered the loss of my mother. Mr. Levin and Mr. Peconti were more than just our lawyers. Words can’t really express our gratitude. My family and I will always be grateful for the compassion that they showed us. I want to thank you for what you did for my family, and for always being there for us.
Margaret’s representation, guidance, and professionalism gave us the sense that we could put our trust in Levin & Perconti and the final outcome proved that to be true.
Legally Reviewed by

Dov Apfel
Contact Us
- Free Consultation
- (312) 332-2872
Related Pages
- Birth Injury Lawyer
- Birth Asphyxia
- Brachial Plexus Injury
- Breech Birth Complications
- Cerebral Palsy
- Erb's Palsy
- Gestational Diabetes Misdiagnosis
- Hypoxic-Ischemic Encephalopathy (HIE)
- Neonatal Seizures
- Oxygen Deprivation
- Preeclampsia Misdiagnosis
- Shoulder Dystocia
- Statute of Limitations by State
- Stillbirth Lawsuit
- Umbilical Cord Compression
- Untimely C-Section
- Vacuum Extraction Injury
Notable Results
SETTLEMENT
for the family of a child who suffered brain injury due to lack of oxygen during her birth
SETTLEMENT
for a child who suffered brain damage causing cerebral palsy as a result of a family practice physician's failure to perform a timely C-section
VERDICT
for a child who died as a result of a doctor’s failure to diagnose the mother with an immune disorder while pregnant
Our Office
325 N LaSalle Dr Suite 300
Chicago, IL 60654
312-332-2872